Imaging Findings:
Hallmark imaging findings in pancreaticoportal fistula include:
1. Changes of acute or chronic pancreatitis.
2. Diffuse fluid-like appearance of the expanded portal-venous system.
- CT – Diffuse fluid-like low attenuation of the portal veins. The density is much lower than expected for bland acute thrombus.
- MR – Diffuse fluid-like T2 hyperintense signal of the portal veins.
T2 hyperintensity is much brighter than expected for acute thrombus.
3. Direct communication of the pancreatic duct and/or a pseudocyst with the portal-venous system.
- Migration of a calculus from the pancreatic duct into the portal venous system can also be seen.
The diagnosis of pancreaticoportal fistula on any imaging modality (CT,
MRI/MCRP,
or ERCP) must demonstrate these findings,
independently or in conjunction with one another.
Example Cases:
Patient 1 (Figures 1-6) is a 61 year old male with chronic alcohol abuse and recurrent pancreatitis. His initial presentation was with abdominal pain.
Imaging work-up revealed communication of the pancreatic duct with the portal venous system. This was visualized on both CT and MRI,
and confirmed with ERCP. Percutaneous drainage of the pseudocyst was performed and the patient abstained from further alcohol use.
Migration of a pancreatic ductal calculus into the superior mesenteric vein was seen on long term follow up imaging.
Follow-up images also demonstrate cavernous transformation of the portal venous system.

Fig. 1: Patient 1. Contrast enhanced axial CT images from 4/2008 demonstrate changes of chronic pancreatitis with parenchymal calcifications in the pancreatic head (yellow arrow), prominence of the pancreatic duct (red arrow), and a calculus within the pancreatic duct (blue arrow). Note patency of the superior mesenteric vein (green arrow).

Fig. 2: Patient 1. Contrast enhanced axial CT images from 9/2009 demonstrate new fluid density within the portal venous system (red arrow) extending to the splenic vein and superior mesenteric vein (white arrow). Note the communication between the pancreatic head pseudocyst containing the calculus (green arrow) with the splenic vein (yellow arrow).

Fig. 3: Patient 1. T2 weighted axial MR image from 9/2009 shows the pancreatic pseudocyst communicating with the splenic vein (red arrow).
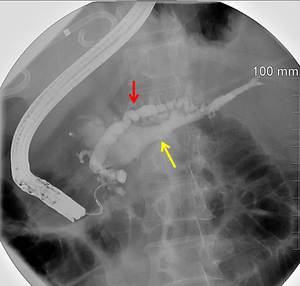
Fig. 4: Patient 1. Single ERCP image from 3/2010 illustrates changes of chronic pancreatitis, with beaded dilatation of the pancreatic duct (red arrow), and opacification of the portal venous system (yellow arrow denotes opacification of the splenic vein). Note also the pigtail catheter draining the large pancreatic pseudocyst.

Fig. 5: Patient 1. Contrast enhanced axial cine CT images from 4/2010 showing progression of pancreatitis with increasing free fluid and a large epigastric pseudocyst. There is increased pancreatic ductal dilatation communicating with the pancreatic head psueducyst. This pseudocyst also communicates with the portal, splenic, and superior mesenteric veins. Note that the calculus previously seen in the pancreatic head pseudocyst has migrated to the superior mesenteric vein, proving a fistulous communication.
Patient 2 (Figures 7-10) is a 55 year old female who presented initially to the emergency department with abdominal pain. Her initial imaging showed changes of acute pancreatitis (Fig.
7).
On follow up imaging,
the patient developed a pancreatic pseudocyst which communicated with the portal venous system (Fig.
8 -10).

Fig. 7: Patient 2. Contrast enhanced axial CT image from 12/2007 demonstrates acute pancreatitis with peripancreatic inflammatory changes.

Fig. 8: Patient 2. Contrast enhanced axial CT images from 12/2010 demonstrate a prominent pancreatic pseudocyst with fluid density within the portal venous system (green arrow). There is a communication between the pseudocyst and the portal vein (red arrow) as well as the pseudocyst and the splenic vein (yellow arrow).

Fig. 9: Patient 2. Single coronal T2 weighted MRCP image from 12/2010 again illustrates the pancreatic pseudocyst and its communications with the portal vein (red arrow) and the portal venous confluence/ splenic vein (yellow arrow).

Fig. 10: Patient 2. Contrast enhanced axial CT images from 2/2011 showing similar findings of the pancreatic pseudocyst in communication with the portal and splenic veins with hypodense contents within the portal and splenic veins
Patient 3 (Figures 11-12) ) is a 25 year old female with a history of polysubstance and alcohol abuse who initially presented with abdominal pain. Preliminary CT images showed changes of acute pancreatitis (Fig.
11 A & B) with development of a pseudocyst on follow up scans (Fig.
11 C & D).
A fistulous communication between pancreatic duct and portal venous system was seen on a subsequent CT scan (Fig.
12).

Fig. 11: Patient 3. Contrast enhanced CT images in a single patient with acute pancreatitis. A) Axial and B) coronal CT images from 12/2010 demonstrate changes of acute pancreatitis with peripancreatic inflammatory stranding. C) Axial and D) coronal CT images from 10/2011 show persistent acute pancreatitis changes with pseudocyst formation (red arrow). The pancreatitc duct is also dilated (yellow arrow).

Fig. 12: Patient 3. Contrast enhanced axial and coronal CT images from 5/2012 demonstrate the interval development of multiple pseudocysts (red arrows). There is new hypodensity within the expanded portal venous system (white arrow), which is contiguous with one of the pseudocysts (yellow arrow).
Patient 4(Figures 13-14) is a 52 year old male who presented with abdomen pain to the emergency department in 2005. At that time,
his CT findings were consistent with acute pancreatitis (Fig.
13 A). He had several recurrent episodes of acute pancreatitis,
and CT in 2008 showed a cystic area in the pancreatic head,
likely representing a pseudocyst (Fig.
13 B). A follow up CT study in 2012 showed changes of chronic pancreatitis (dilated pancreatic duct and calcifications) and a growing cystic lesion in the pancreatic head (Fig.
13 C & D).
Communication of this cystic lesion with splenic vein as well as hypodense material in the portal venous system was noted,
suggesting pancreaticoportal fistula (Fig.
14). Chronic changes of cavernous transformation of portal vein are also present (Fig.
14).

Fig. 13: Patient 4. Serial contrast enhanced axial CT images demonstrate pancreatic and peripancreatic changes in a single patient over the course of time. A) Single image from 8/2005 shows findings of acute pancreatitis with peripancreatic inflammatory changes. B) Single image from 10/2008 illustrates a pancreatic head pseudocyst (red arrow). C-D) Images from 5/2012 show an enlarging pancreatic head pseudocyst and other changes of chronic pancreatitis, including pancreatic ductal dilatation and parenchymal calcifications.

Fig. 14: Patient 4. Contrast enhanced axial and coronal CT images from 11/2012 demonstrate pancreatic pseudocyst communicating with the portal venous system (red arrow). There is hypodense content within the portal venous system (white arrow). The pseudocyst also communicates with the pancreatic duct (yellow arrow). There is cavernous transformation of the portal vein (green arrow). Incidentally noted are bilateral renal solid and cystic lesions.




























